Seeking Social Justice for Childbearing Women Through Legislative Advocacy
BY CINDY L. FARLEY, CNM, PH.D., FACNM, LINDSAY DORSEY, BSN, SNM, & KATIE DANIELSON, BSN, SNM | May 3, 2018
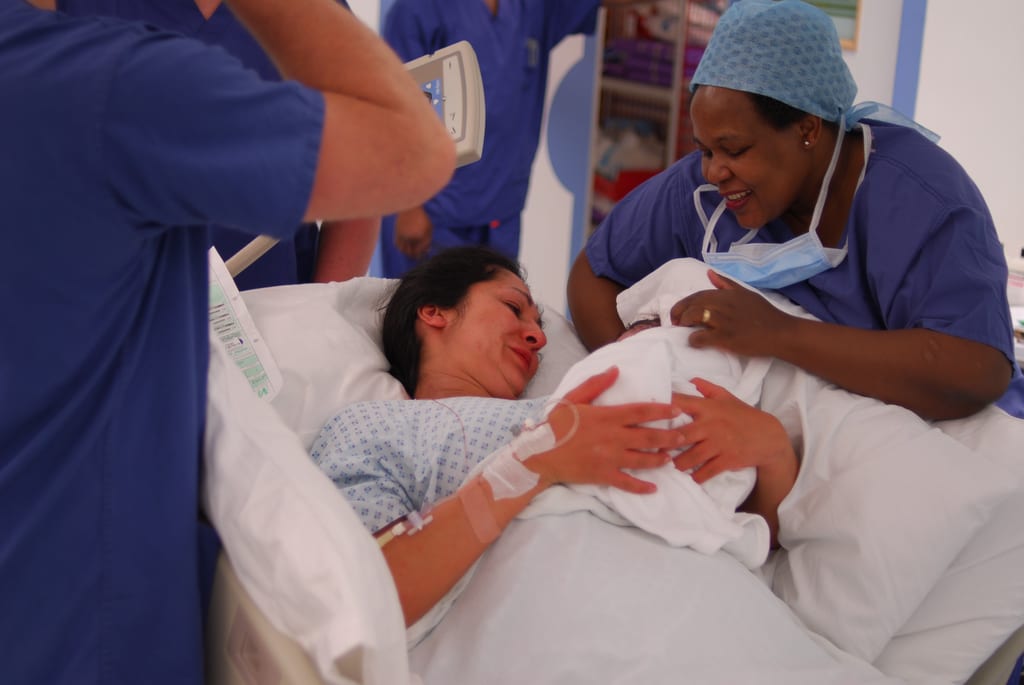
Childbearing women today face a number of social inequities in the United States. More than 40% of US counties have no maternity care provider. Urban and rural hospitals are closing labor and birth units, especially impacting services to women of color and women with limited financial or social resources. Mismatches often exist between the payment method a pregnant woman has and the local practices that will accept her reimbursement, leading to restricted choices or financial hardships. Racial and ethnic groups, such as African-American women and Hispanic women, experience higher rates of infant and maternal morbidity and mortality compared to Caucasian women. In spite of spending the most money per individual for healthcare, the United States is the only developed nation that is experiencing a rise in maternal death, a tragedy that occurs to more than two women in this country every 24 hours. Labor and birth care is dominated by technology and surgery, overshadowing essential humanistic care that facilitates physiologic birth, such as offering therapeutic presence and compassionate support. Yet physiologic birth is not only less costly but more likely to preserve a woman and her child’s health.
These complex problems have multiple causes. Solutions must come through a variety of approaches. Political advocacy for equity and justice through legislation and health policy is one important approach. The Ignatian value of social justice includes an emphasis on education and action as men and women for others and is in concert with legislative advocacy efforts.
Georgetown University via Salim Fadhley/flickr
Midwives and Women’s Health Nurse Practitioners (WHNPs) are healthcare professionals deeply committed to providing compassionate, evidence-based care to women across the lifespan, and particularly to childbearing women and their families. The Nurse-Midwifery and WHNP education programs at Georgetown University changed their master’s degree offered on campus to a hybrid online format in 2011. Students have small, synchronous classes with faculty via virtual classrooms, allowing presentation, discussion, engagement, and connection. The courses are web-based and include objectives, readings, webcast lectures, and other resources. Students learn to provide care for women usually in their locale, often in small towns, medically underserved urban sites, or rural areas. The move to an online format has opened the opportunity to receive a rigorous, values-based Jesuit education to students who were otherwise place-bound. Students from various states come to campus three times during their seven-term program for intensive simulation learning of clinical skills, seminar discussions applying Jesuit values to real-world issues, and experiential learning activities, such as learning advocacy skills on Capitol Hill.

Dr. Cindy Farley (OH) and Lindsay Dorsey (PA) outside Senator Robert P. Casey, Jr.’s DC Office
The Nurse-Midwifery and Women’s Health Nurse Practitioner (WHNP) curriculum at Georgetown University includes discussion about legislative initiatives that focus on midwifery and women’s health. The specific initiatives facilitate an appreciation of the influence of law and policy on women’s experiences and outcomes and on the healthcare system as a whole. Students then develop skills in communicating the value of midwifery and women’s health care to legislators and other stakeholders through in-person visits to their federal legislators: two Senators and one Congressperson. With its geographic location in Washington, D.C., Georgetown University is ideally situated to provide powerful experiential learning in social justice through advocacy efforts.
Legislative “asks” must meet two criteria and be: 1) consistent with Georgetown values and 2) supported by the American College of Nurse-Midwives and the Nurse Practitioners in Women’s Health, the relevant national professional organizations. For the January 2018 visits, advocacy efforts were directed toward:
- Improving Access to Maternity Care (S. 783)
- Preventing Maternal Deaths Act of 2017 (H.R.1318/S. 1112)
- Addiction Treatment Access Improvement Act (H.R. 3692).
Students are universally nervous before the visits, yet confident and positive afterward. A debriefing occurs that enables students to share their stories with their classmates and faculty. The stories from two students illustrate anecdotes about visiting their federal legislators.
Lindsay Dorsey:
Preparing for Capitol Hill was unnerving to say the least. Never considering myself to be political, I had no interest and thought it would not benefit me at all in becoming a Certified Nurse-Midwife/Women’s Health Nurse Practitioner. The night before, one of my classmates and I practiced our introductions and talking points in preparation for the next day.
Arriving at the Dirksen Senate Office Building, we gave each other the “I can’t believe we are still doing this” look. Once inside, seated and being prepared to meet with our legislators or staff members, the importance of the day took over and I pulled out my notes to be sure I remembered my talking points. Sitting at the table with my federal legislative staff members was an experience that I will never forget. I was there to discuss the introduction of laws that can improve outcomes for maternal and infant health in my community and throughout the United States. My voice had the power to change laws and even if those changes didn’t occur immediately, a seed was planted. I had a wonderful experience and I knew going forward that my newfound sense of empowerment would absolutely make me a better provider and advocate for the women I will serve.

Dr. Farley and Lindsey Dorsey on the Senate building underground train.
Katie Danielson:
In January, my Georgetown classmates and I met with our federal legislators. We spoke about who we were as professionals and why our work is essential to women’s health.

Kelsey Sour (MN), Katie Danielson (MN), Deborah Landes (CA), and Spring Maddox (CA) storm the Hill during a winter storm on January 4, 2018.
We advocated for their support on selected bills, highlighting the impact on the health and well-being of women and their families in our districts. For example, in my district, there are no certified nurse-midwives despite the community need and desire for them. I spoke about the importance of increased access to primary care providers and the role that midwives and nurse practitioners have in helping to meet women’s healthcare needs.
Post-graduation, I am considering opening a birth center where care for healthy childbearing women is provided within a wellness model. I need to be aware of legislation and regulation that affect what I can and cannot do in establishing this service. Having the tools to effectively communicate with those in office is essential to move towards an environment where midwives and nurse practitioners can practice to their fullest potential and do the most good.
Guest bloggers:
Cindy L. Farley, CNM, PhD, FACNM, is an Associate Professor in Georgetown University’s distance learning Nurse-Midwifery/Women’s Health Nurse Practitioner programs. She lives in Yellow Springs, Ohio and does locum tenen work with the Amish women of Holmes and Stark Counties in Ohio.
Lindsay Dorsey, RN, BSN, is a graduate student at Georgetown University in the Certified Nurse Midwife/Women’s Health Nurse Practitioner program. She currently resides in Philadelphia, Pa with her two children, 13 and 7 years of age.
Katie Danielson, RN, BSN is a recent graduate of Georgetown University’s Nurse-Midwifery and Women’s Health Nurse Practitioner programs. She currently resides in Bemidji, MN with her husband and 4 children. She is active as a student legislative contact and as a student Governmental Affairs Committee member with the American College of Nurse-Midwives.
ISN welcomes faith & justice related blog submissions from members of the Ignatian family. Please let us know of any blog ideas or posts using this form: ISN Blog Ideas







Women – they are the pillars of humanity.